Questionable convictions in “shaken baby” cases
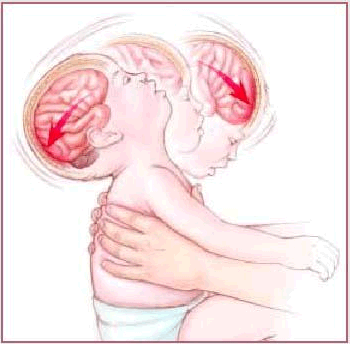
The term “shaken baby syndrome” (SBS) was developed to explain those instances in which severe intracranial trauma occurred in the absence of signs of external head trauma. SBS is the severe intentional application of violent force (shaking) in one or more episodes, resulting in intracranial injuries to the child. Physical abuse of children by shaking…
Read More